| Table of Contents |  |
|
Case Report
| ||||||
| Co-existence of nocardiosis with pulmonary aspergillosis in a single patient | ||||||
| Gunjan Garg1, Pratyush Miglani2, Ambuj Garg3, Agarwal PK4 | ||||||
|
1MBBS, Post Graduate Student (Internal Medicine), Department of Internal Medicine, Sir Ganga Ram Hospital, New Delhi, Delhi, India.
2MBBS, MD, Senior Resident, Department of Internal Medicine, Sir Ganga Ram Hospital, New Delhi, Delhi, India. 3MBBS, DNB, Associate Consultant, Department of Internal Medicine, Sir Ganga Ram Hospital, New Delhi, Delhi, India. 4MBBS, MD, Senior consultant, Department of Internal Medicine, Sir Ganga Ram Hospital, New Delhi, Delhi, India. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Garg G, Miglani P, Garg A, Agarwal PK. Co-existence of nocardiosis with pulmonary aspergillosis in a single patient. Edorium J Med 2014;1:1–3. |
|
Abstract
|
|
Introduction:
Nocardia and Aspergillus are important causes of opportunistic infections in immunocompromised individuals. An aggressive workup is essential since these infections are remediable but potentially mortal.
Case Report: We describe a case of a 50-year-old diabetic female with pulmonary aspergillosis who presented with cough and breathlessness for one and ahalf months. She was given steroids and itraconazole for the same but there was no relief. Later on, Bronchoalveolar lavage on Kinyoun stain showed Nocardia. Conclusion: This case highlights the importance to look for other causes as well in patients with pulmonary aspergillosis not responding to treatment since delay in diagnosis can be fatal for the patient. | |
|
Keywords:
Aspergillus, Nocardia, Diabetes mellitus, Tuberculosis
| |
|
Introduction
| ||||||
|
Pulmonary disease is the common manifestation of infection by Nocardia and Aspergillus and is usually fatal if it goes unrecognized. They are unusual in immunocompetent individuals and co-infection with both is even odder. We report one such case of mixed infection with Nocardia and Aspergillus in a diabetic female. | ||||||
|
Case Report
| ||||||
|
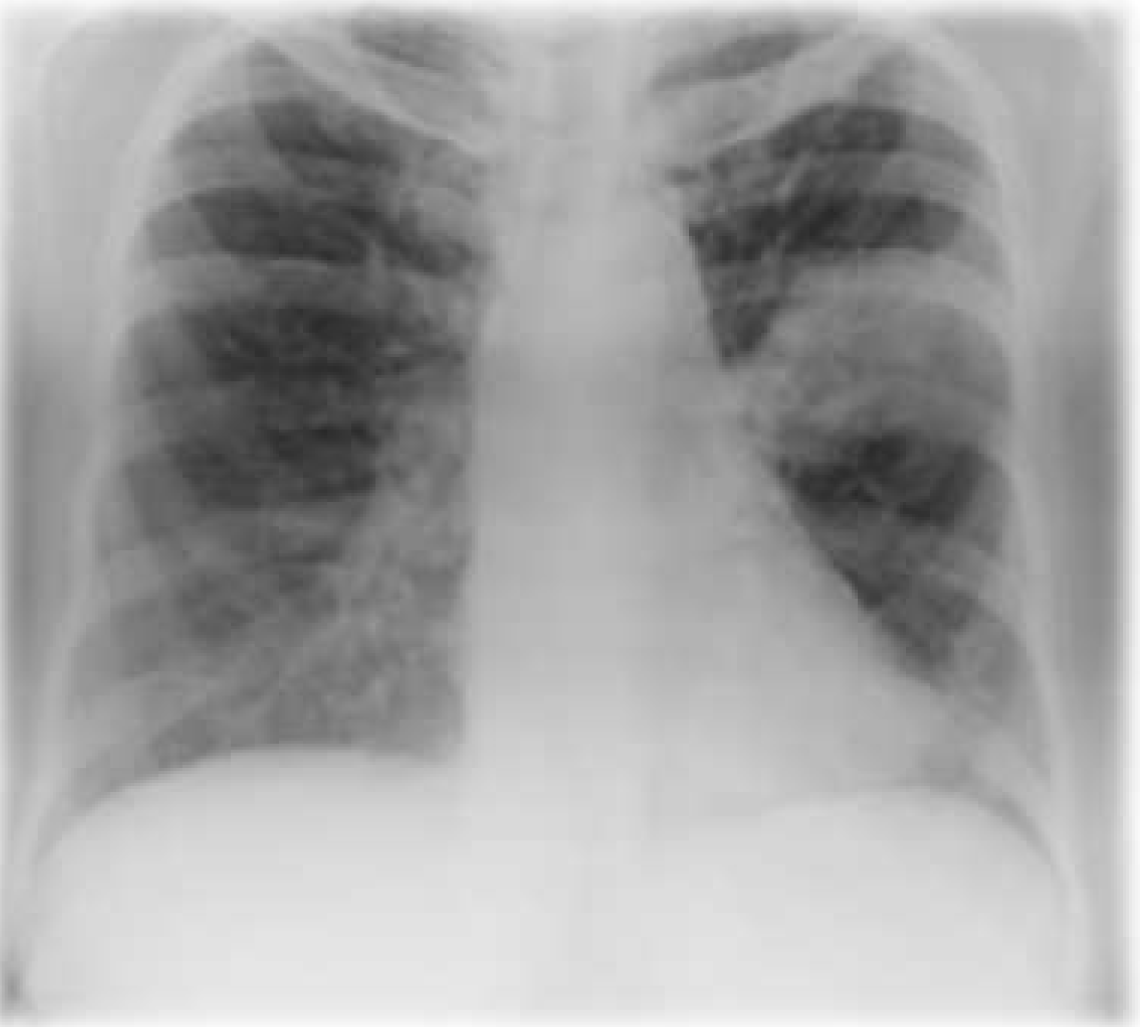
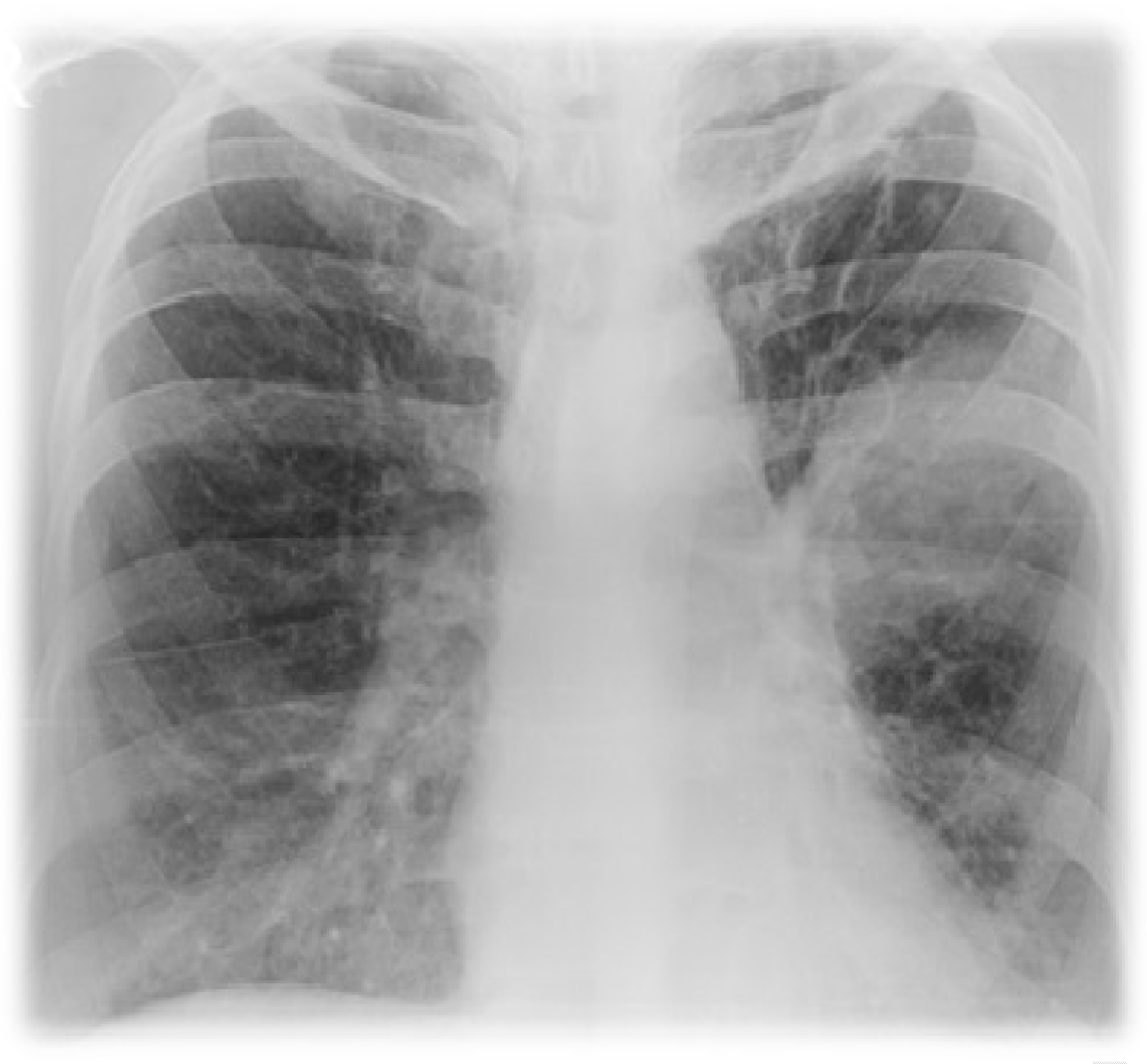
A 50-year-old diabetic female, suffering from post-tubercular bronchiectasis presented with worsening cough and breathlessness over past one and ahalf months. For these ongoing symptoms, she was evaluated elsewhere and diagnosed as pulmonary aspergillosis (serum Immunoglobulin E levels were >2500 IU/mL, absolute eosinophil counts were 1600/mm3, immunoglobulin G anti-Aspergillus titre was >200). She was taking oral glucocorticoids and itraconazole for the same. On hospitalization, she complained of persistent cough with expectoration and breathlessness. Respiratory system examination revealed crepitations in bilateral lung fields. All the laboratory investigations were normal except for glycated hemoglobin which was 8.9%. Microbiological examination of sputum was normal. Chest radiograph (Figure 1) revealed homogeneous opacities in left mid zone and right upper zone. At this stage, she was managed with intravenous antibiotics, oral glucocorticoids and other supportive measures. Follow-up chest X-rays showed increase in the size of left-sided opacity. Contrast-enhanced computed tomography scan of thorax revealed bronchiectasis in bilateral lungs with necrotic consolidation in left upper lobe with infective bronchiectatic segments in right upper lobe and necrotic tree in bud appearance in bilateral lungs. Citing no relief to the patient, bronchoscopy was carried out which was normal. Bronchoalveolar lavage analysis was negative for Gram's, acid-fast bacilli and fungal stain but Kinyoun stain showed growth of Nocardia. The patient was additionally started on oral co-trimoxazole DS twice daily according to sensitivity of organism cultured. By fourth day, she was symptomatically better and her chest X-ray showed resolution of the lesion (Figure 2). Subsequently, the patient was discharged in stable condition with advice for further follow-up. | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Pulmonary aspergillosis is an allergic or hypersensitive reaction to fungus. It is commonly caused by Aspergillus fumigatus. The incidence of aspergillosis has increased with rise in prevalence of immunocompromised patients associated with the management of malignancy, organ transplantation, autoimmune and inflammatory conditions; critically ill patients and those with chronic obstructive pulmonary disease. It is characterized by cough, breathlessness, coughing up thick sputum casts and recurrent transient chest radiographic infiltrates. The diagnostic features include markedly increased total IgE (>1000 IU/mL), positive skin prick test to Aspergillus fumigatus extract or detection of specific IgE and IgG levels [1]. Radiologic features consists of nodules ranging from 1–3 cm which cavitate in 50% of patients [2]. The diagnosis is based upon the presence of a combination of clinical, biological and radiological criteria [3]. Introduction of new non-invasive tests, with more effective and better-tolerated drugs, has resulted in lower mortality rates. Pulmonary nocardiosis is the most common clinical presentation of Nocardia because inhalation is the primary route of bacterial exposure. Majority of patients with pulmonary nocardiosis have identifiable risk factors mainly corticosteroid or other immunosuppressant therapy [4]. It presents with productive or non-productive cough, pleuritic pain, hemoptysis, fever, anorexia, malaise, and weight loss. The chest X-ray findings can be variable, displaying focal or multifocal disease with nodular and/or consolidation infiltrate as well as cavitary lesions [5]. The cavitary lesions in immunodeficient individuals are caused by various organisms besides Nocardia like Staphylococcus aureus, Pseudomonas, Mycobacterium tuberculosis. The cavitary lesion can even masquerade malignancy [6]. Treatment mainly constitutes 10–20 mg/kg of trimethoprim and 50–100 mg/kg of sulfamethoxazole per day, gradually they can be tapered in view of positive clinical response from patient. Sulfonamide resistant Nocardia species can be treated with third generation cephalosporins and imipenem [7]. | ||||||
|
Conclusion
| ||||||
|
The co-existence of aspergillosis and nocardiosis in the same patient is rarely reported in literature. Hence, we emphasize our readers to keep their differential diagnosis wide open while dealing with such cases. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Gunjan Garg – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Pratyush Miglani – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Ambuj Garg – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Agarwal PK – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Gunjan Garg et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|